January 30th is Global Neglected Tropical Diseases (NTD) Day. This is a worldwide campaign to raise awareness of these often-overlooked conditions. World NTD Day serves as a call to action to secure increased resources for neglected tropical diseases, and crucially facilitate political leadership and ownership of NTD programs from affected countries.
The 2021 Neglected Tropic Disease roadmap highlights that 50% of NTDs relate to the skin. When chromoblastomycosis was accepted as an NTD in 2017, it included ‘other deep mycoses’. Amongst these both mycetoma and sporotrichosis are included. Should African histoplasmosis also be added to this list?
Almost all cases of African histoplasmosis are reported from Africa. This debilitating infection is caused by duboisii, a close relative of capsulatum, the fungus that causes disseminated histoplasmosis in AIDS, and is often fatal. African histoplasmosis differs as it causes chronic skin, lymph, and bone infection in people without an immune deficiency and is often seen in older children and younger adults.
There are still many unanswered questions about African histoplasmosis. We do not know enough about the fungus that causes it or the mechanism it uses to enter the human body. It is also unclear as to why it so often travels to the bones and distant parts of the skin. Specific treatment options are also currently unavailable. What is undeniable is that this disease is disfiguring and stigmatising for those affected. It should certainly be an NTD.
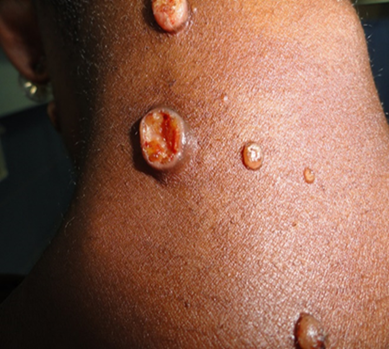
A patient with African histoplasmosis causing ulcerating nodules on the neck. Thanks to Dr. Martin Agyei, Consultant Dermatologist, Komfo Anokye Teaching Hospital, Ghana.
On Global NTD Day, GAFFI highlights the uncommon and enigmatic African histoplasmosis to raise awareness of the condition so those who suffer from the disease don’t go unnoticed and can get the treatment they need.
Professor David Denning from GAFFI and The University of Manchester said:
“African histoplasmosis, like all the skin fungal NTDs, requires a diagnostic cascade of a skin biopsy by a dermatologist or other skilled person, direct microscopy and fungal culture by a well-trained laboratory technologist, and histopathology by an aware pathologist. To improve clinical outcomes, we need these skills widely available in Africa.”
Professor David Denning
A video describing the disease in detail has been recorded by GAFFI’s Ambassador for Ghana, Bright Ocansey, and can be viewed here. Bright declared:
“African histoplasmosis looks like many skin infections including some NTDs common in Africa such as leishmaniasis, Buruli ulcer, and mycetoma. Cases that are diagnosed in the laboratory usually come as a surprise to the clinician. Sending pus or skin biopsy for direct microscopy and histopathologic analysis is very helpful in the hands of a laboratorian/pathologist who ‘thinks fungi’, but, care must be taken to avoid confusion with other endemic mycoses.”
Bright Ocansey
#WorldNTDDay2022
#BeatNTDs